Dr. Michael Skinner coauthored a 2021 review arguing for inclusion of epigenetic transgenerational inheritance into evolutionary theory:
“Over the past 50 years, molecular technology has been used to investigate evolutionary biology. Many examples of finding no correlated genetic mutations or a low frequency of DNA sequence mutations suggest that additional mechanisms are also involved.
- Identical twins have essentially the same genetics, but generally develop discordant disease as they age.
- Only a low frequency (generally 1% or less) of individuals that have a specific disease have a correlated genetic mutation.
- Dramatic increases in disease frequency in the population cannot be explained with genetics alone.
DNA methylation, histone modifications, changes to chromatin structure, expression of non-coding RNA, and RNA methylation can directly regulate gene expression independent of DNA sequence. These different epigenetic factors do not only act independently, but integrate with each other to provide a level of epigenetic complexity to accommodate the needs of cellular development and differentiation.
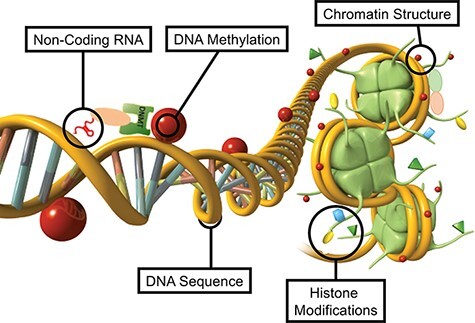
Environmental epigenetics is the primary molecular mechanism in any organism that is used to promote physiological and phenotypic alterations. Actions of environmental factors early in development can permanently program the cellular molecular function, which then impacts later life disease or phenotypes.

Integration of epigenetics and genetics contribute to a Unified Theory of Evolution that explains environmental impacts, phenotypic variation, genetic variation, and adaptation that natural selection acts on. The current review expands this proposed concept and provides a significant amount of supporting literature and experimental models to support the role of environmentally induced epigenetic transgenerational inheritance in evolution.”
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8557805/ “Role of environmentally induced epigenetic transgenerational inheritance in evolutionary biology: Unified Evolution Theory”
Organisms cited in this review’s references are similar to humans in ancestral influences and developmental influences during the first 1000 days of our lives. Humans are different in that even after all these influences, we can choose to influence our own change and individually evolve. We can also change our internal environments per Switch on your Nrf2 signaling pathway and An environmental signaling paradigm of aging.











 Living beings – thousands of years old – living together
Living beings – thousands of years old – living together

