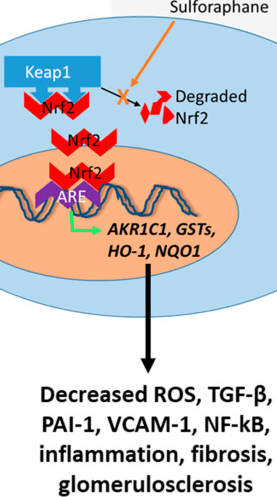
Here are thirty 2019 and 2020 papers related to Switch on your Nrf2 signaling pathway topics. Started gathering research on this particular theme three months ago.
There are more researchers alive today than in the sum of all history, and they’re publishing. I can’t keep up with the torrent of interesting papers.

2019 Polyphenols and Intestinal Permeability: Rationale and Future Perspectives
2020 Prebiotic effect of dietary polyphenols: A systematic review
2019 Protease‐activated receptor signaling in intestinal permeability regulation
2019 Intestinal epithelial cells: at the interface of the microbiota and mucosal immunity
2020 The Immature Gut Barrier and Its Importance in Establishing Immunity in Newborn Mammals
2019 Prebiotics and the Modulation on the Microbiota-GALT-Brain Axis
2019 Prebiotics, Probiotics, and Bacterial Infections
2020 Vitamin D Modulates Intestinal Microbiota in Inflammatory Bowel Diseases
2020 Microbial tryptophan metabolites regulate gut barrier function via the aryl hydrocarbon receptor
2019 Involvement of Astrocytes in the Process of Metabolic Syndrome
2020 Intestinal Bacteria Maintain Adult Enteric Nervous System and Nitrergic Neurons via Toll-like Receptor 2-induced Neurogenesis in Mice (not freely available)
2020 Plasticity of Paneth cells and their ability to regulate intestinal stem cells
2020 Shaping the Innate Immune Response by Dietary Glucans: Any Role in the Control of Cancer?
2020 Systemic microbial TLR2 agonists induce neurodegeneration in Alzheimer’s disease mice
2020 Effectiveness of probiotics, prebiotics, and prebiotic‐like components in common functional foods
2020 Postbiotics-A Step Beyond Pre- and Probiotics
2019 Pain regulation by gut microbiota: molecular mechanisms and therapeutic potential
2020 Postbiotics: Metabolites and mechanisms involved in microbiota-host interactions
2020 Postbiotics against Pathogens Commonly Involved in Pediatric Infectious Diseases
2019 Glutamatergic Signaling Along The Microbiota-Gut-Brain Axis
2019 Health Benefits of Heat-Killed (Tyndallized) Probiotics: An Overview
2020 New Horizons in Microbiota and Metabolic Health Research (not freely available)



 Surface! Surface! Surface!
Surface! Surface! Surface!