Two 2021 reviews presented aspects of human immune systems:
“The adaptive immune system’s challenge is to protect the host through generation and differentiation of pathogen‐specific short‐lived effector T cells, while in parallel developing long‐lived memory cells to control future encounters with the same pathogen.
The system highly relies on self‐renewal of naïve and memory T cells, which is robust, but eventually fails. Genetic and epigenetic modifications contribute to functional differences in responsiveness and differentiation potential.
Less than 20% of nascent T cells are produced from the thymus in young adults, which dwindles to less than 1% after the age of 50 years. Even in young adults, the majority of T cells are produced in the periphery. A pickup in proliferation has been described in late life, possibly as a consequence of increased cell death and evolving lymphopenia.
One challenge of the aging process is to replenish cells while keeping integrity of the organ. The dynamic lymphoid system employs a vast number of T cells (>1011) and maintains a balance between cell production, death, and differentiation.
Enormous TCR ( T cell receptor) diversity is required to be able to respond to the universe of possible peptides (>209). Only T cell generation in the thymus can add new TCR specificities. Homoeostatic proliferation at best maintains diversity, >108 unique TCRs in a given adult.
Antigen-specific memory T cells adopt several fates with age:
- Decrease in stem-like memory T cells;
- Increase in NK (natural killer) cell-like TEMRA (terminally differentiated effector T cells);
- Increase in exhausted T cells;
- Increase in short-lived effector memory T cells; and
- Decrease in tissue-residing T memory cells.
Virtual memory T cells without prior experience of antigen encounter also increase with age.”
https://febs.onlinelibrary.wiley.com/doi/epdf/10.1111/febs.15770 “Hallmarks of the aging T cell system”
“Trained immunity is characterized by long‐term functional reprogramming of innate immune cells following challenge with pathogens or microbial ligands during infection or vaccination. This cellular reprogramming leads to increased responsiveness upon re‐stimulation, and is mediated through epigenetic and metabolic modifications.
Trained immunity has been shown to last for at least 3 months and up to 1 year, while heterologous protection against infections can last for at least 5 years. These long-term effects are mediated through reprogramming of myeloid progenitor cells in bone marrow, which in turn generate myeloid cells with a trained immunity phenotype.
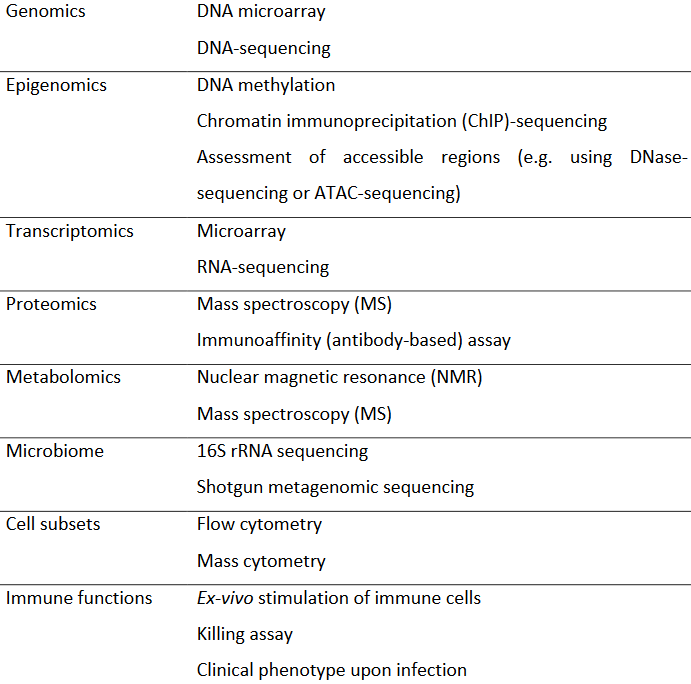
Molecular mechanisms underlying trained immunity, for example induced by β-glucan or Bacille Calmette‐Guérin (BCG) vaccination, can be investigated by using and integrating different layers of information, including genome, epigenome, transcriptome, proteome, metabolome, microbiome, immune cell phenotyping and function. Interplay between epigenetic and metabolic reprogramming is necessary for induction of trained immunity, as certain metabolites have a direct effect on enzymes involved in epigenetic remodeling.
High-throughput methods allow researchers to use an unbiased approach examining many potential genes or markers in relation to health and disease, rather than examining a limited number of candidate genes or markers.
One strength of integrating multiple levels of data is an increased power to identify key regulatory molecular networks driving trained immunity. For example, results obtained from one level (i.e. genes) can be used to reduce the number of traits to test in a second level (i.e. proteins), thereby increasing power.
One important pitfall when it comes to designing effective omics studies, is sample size. With a large number of markers measured, and the relatively small contributing effect size of individual analytes, the risks of both type 1 and 2 errors are high without sufficient sample sizes for both discovery and validation cohorts.”
https://onlinelibrary.wiley.com/doi/pdf/10.1002/eji.202048882 “Resolving trained immunity with systems biology”