Three papers on gut barriers, with the first a 2020 review of four intestinal barrier layers:
“The epithelial cell layer and outer/inner mucin layer constitute the physical barrier. Intestinal alkaline phosphatase (IAP) produced by epithelial cells and antibacterial proteins secreted by Paneth cells represent the functional barrier.
Multiple layers of this barrier, from intestinal lumen to systemic circulation, include:
- Luminal intestinal alkaline phosphatase (IAP) that dephosphorylates bacterial endotoxin lipopolysaccharide (LPS) to detoxify it;
- Mucus layer that provides a physical barrier preventing interactions between gut bacteria and intestinal epithelial cells;
- Tight junctions between epithelial cells that limit paracellular transport of bacteria and/or bacterial products to systemic circulation; and
- Antibacterial proteins secreted by specialized intestinal epithelial cells or Paneth cells, and IgA [immunoglobulin A] secreted by immune cells present in lamina propria underlying the epithelial cell layer.

The presence of LPS in systemic circulation is identified as a causal or complicating factor in diverse diseases such as:
- Diet-induced metabolic diseases;
- Autism;
- Alzheimer’s disease;
- Parkinson’s disease;
- Arthritis;
- Obesity-induced osteoarthritis;
- Asthma; and
- Several autoimmune diseases.
Causal relationships between circulating LPS levels and development of multiple diseases underscore the importance of changes in intestinal barrier layers associated with disease development.
Correcting intestinal barrier dysfunction to modulate multiple diseases can be envisioned as a viable therapeutic option. Identifying precise defects by use of specific biomarkers would facilitate targeted interventions.”
https://academic.oup.com/jes/article/4/2/bvz039/5741771 “Intestinal Barrier Dysfunction, LPS Translocation, and Disease Development”
A second 2020 review focused on IAP:
“IAP plays a vital role in intestinal barrier function, affecting bicarbonate secretion, duodenal surface pH, nutrient resorption, local intestinal inflammation, and gut microbiota. Disturbances of IAP functions are associated with persistent inflammatory diseases associated with aging (i.e.,inflammageing), inflammatory bowel diseases, type 2 diabetes mellitus, obesity, metabolic syndrome, and chronic kidney disease (CKD).
Expression and activity of IAP are directly affected by food intake, i.e., quantity and type of macro- and micronutrients including vitamins and other bioactive nutrients, or by absence of food, as well as indirectly by composition of gut microbiota that in turn are highly dependent on food intake. Increased IAP gene expression and activity promoting detoxification of LPS may lead to improvement of both intestinal and systemic inflammation, reduced bacteria translocation, and maintaining gut barrier function.
IAP could be used as an inflammatory marker together with other markers, such as interleukins, to predict inflammation and diseases that are based on chronic inflammatory processes.”
https://doi.org/10.1007/s13167-020-00228-9 “Intestinal alkaline phosphatase modulation by food components: predictive, preventive, and personalized strategies for novel treatment options in chronic kidney disease” (not freely available)
A third paper was a 2021 rodent study by coauthors of the first paper:
“We developed intestine-specific IAP transgenic mice (IAPTg) overexpressing human chimeric IAP to examine direct effects of increased IAP expression on barrier function and development of metabolic diseases. We evaluated effects of intestine-specific IAP overexpression in hyperlipidemic Ldlr−/− mice. The data presented demonstrated significant attenuation of Western-type diet (WD)-induced LPS translocation in Ldlr−/−IAPTg mice, with significant reduction in intestinal lipid absorption, hyperlipidemia, hepatic lipids, and development of atherosclerotic lesions.
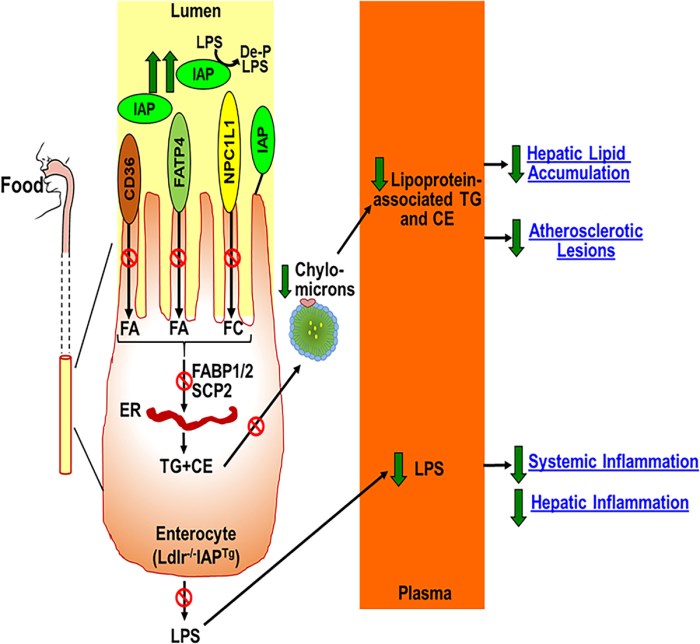
IAP is produced by enterocytes, and catalyzes removal of 1 of the 2 phosphate groups from the toxic lipid A moiety of LPS. This produces monophosphoryl-LPS, and results in attenuation of the downstream TLR (Toll-like receptor)-4–dependent inflammatory cascade.
IAP also:
- Dephosphorylates other proinflammatory molecules such as flagellin and ATP, resulting in their detoxification;
- Regulates expression of key gap junction proteins (zonula occludens, claudin, and occludin) and their cellular localization, which directly modulates intestinal barrier function;
- Promotes growth of various commensal bacteria in the gut by decreasing luminal concentrations of nucleotide triphosphates via dephosphorylation; and
- Translocates from the apical surface of enterocytes during fat absorption. Increased serum IAP accompanies fat absorption, which is consistent with observed increased levels of circulating LPS in WD-fed mice, providing one more likely mechanism by which WD affects intestinal barrier function via IAP.
Nutrients and food components/supplements that increase IAP include galacto- or chito- oligosaccharides, glucomannan, and vitamin D3. These provide a novel opportunity to develop simple strategies for modulation of diet/nutrition to target metabolic diseases including diabetes, fatty liver disease, atherosclerosis, and heart disease.”
https://www.ahajournals.org/doi/10.1161/CIRCRESAHA.120.317144 “Over-Expression of Intestinal Alkaline Phosphatase Attenuates Atherosclerosis”
Previously curated IAP studies were: