I haven’t mentioned α-ketoglutarate for a while, although I’ve taken it twice a day for several years. Here are four 2025 papers on α-ketoglutarate, starting with a review of its role in bone health:
“α-Ketoglutarate (α-KG) serves as a pivotal intermediate in various metabolic pathways in mammals, significantly contributing to cellular energy metabolism, amino acid metabolism, and other physiological processes. α-KG may be a therapeutic target for a variety of bone-related diseases, such as osteoporosis, osteoarthritis, and rheumatoid arthritis, because of its role in maintaining metabolic balance of bone.
α-KG, as a rate-determining mitochondrial intermediate, is crucial in cell energy metabolism because it connects intracellular carbon and nitrogen metabolism between isocitrate and succinyl coenzyme A. Additionally, α-KG is closely involved in the amino acid cycle. As a precursor of amino acids such as glutamine and glutamic acid, α-KG plays a direct role in energy production and a wide range of cellular chemical reactions. α-KG provides an energy source, stimulating protein synthesis, inhibiting protein degradation in muscle, and serving as a significant metabolic fuel for gastrointestinal cells.
α-KG promotes osteogenic differentiation of stem cells, increases activity of osteoblasts to promote osteogenesis, and inhibits bone resorption activity of osteoclasts. α-KG in articular cartilage promotes differentiation and maturation of chondrocytes and formation of a cartilage matrix. The protective effect of α-KG on bone has practical value in treatment of abnormal bone loss symptoms in various bone tissue diseases.”
https://www.sciengine.com/ABBS/doi/10.3724/abbs.2025020 “Essential role of the metabolite α-ketoglutarate in bone tissue and bone-related diseases”
A rodent study explored adding α-KG to osteoarthritis treatment:
“Mesenchymal stem cell (MSC) therapy represents a promising treatment strategy for osteoarthritis (OA). Nevertheless, the therapeutic efficacy of MSCs may be attenuated under conditions of cellular senescence or when the available clinical quantity is insufficient. α-Ketoglutarate (AKG) exerts beneficial effects on skeletal tissues and activity of stem cells. The present study was designed to explore the potential of AKG in augmenting viability of MSCs and the potential of their combined utilization in treatment of OA.
AKG plays a crucial role in multiple biological processes. It is involved in regulating stem cell differentiation, exerts anti-apoptotic effects, modulates the body’s immune and inflammatory responses, contributes to muscle and bone development, and is essential for maintaining stability of the cartilage matrix.
Platelet-rich plasma (PRP) has been demonstrated to have protective effects on chondrocytes and can effectively repair damaged cartilage in OA. However, PRP has intractable problems in terms of product quality control and allogeneic application, and its long-term therapeutic effect gradually weakens.
Combining AKG’s regulation of cellular metabolism with the multi-directional differentiation and immunomodulatory functions of MSCs is likely to generate a synergistic effect. This combined treatment modality targets the complex pathological processes of OA, including cartilage damage, inflammatory responses, and extracellular matrix imbalance, in a more comprehensive manner than a single therapy.”
https://www.sciencedirect.com/science/article/pii/S2707368825000032 “The repair effect of α-ketoglutarate combined with mesenchymal stem cells on osteoarthritis via the hedgehog protein pathway”
A rodent study investigated whether α-KG has a role in determining frailty:
“Frailty is an age-related geriatric syndrome, for which the mechanisms remain largely unknown. We performed a longitudinal study of aging female (n = 40) and male (n = 47) C57BL/6NIA mice, measured frailty index, and derived metabolomics data from plasma samples.
We find that frailty related metabolites are enriched for amino acid metabolism and metabolism of cofactors and vitamins, include ergothioneine, tryptophan, and alpha-ketoglutarate, and present sex dimorphism. We identify B vitamin metabolism related flavin adenine dinucleotide and pyridoxate as female-specific frailty biomarkers, and lipid metabolism related sphingomyelins, glycerophosphoethanolamine and glycerophosphocholine as male-specific frailty biomarkers.
We were interested to observe whether metabolite abundance at any specific timepoint was associated with frailty at a future timepoint. Unfortunately, we didn’t observe any metabolites that showed an overall significant association with future FI (FIf) or future devFI (devFIf). When focusing only on the abundance of metabolites at the baseline time point (∼400 days), we found a single metabolite, alpha-ketoglutarate, was negatively associated with both FIf and devFIf.”
https://www.biorxiv.org/content/10.1101/2025.01.22.634160v1.full “Metabolomics biomarkers of frailty: a longitudinal study of aging female and male mice”
Wrapping up with a rodent study adding α-KG to exercise for its effects on depression and learning:
“aKG acts as a prophylactic and antidepressant to effectively counteract social avoidance behaviors by modulating BDNF levels in the hippocampus and nucleus accumbens. Exercise increases aKG levels in the circulation.
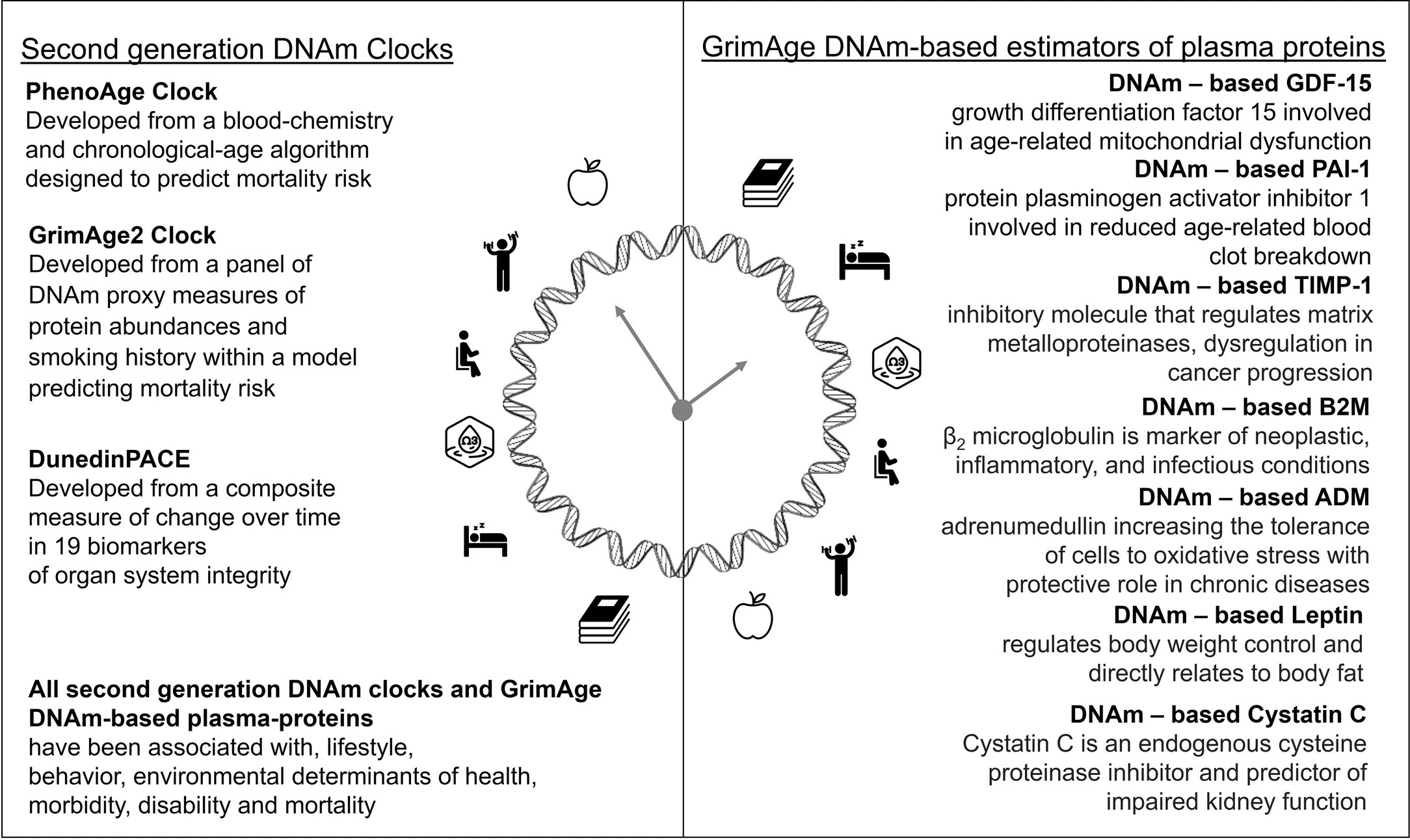
In mice, aKG supplementation prolongs lifespan and reduces aging-associated frailty. aKG supplementation also reverses aging in humans as measured by DNA methylation patterns.
aKG functions as a co-factor for epigenetic enzymes. Changes in the intracellular αKG/succinate ratio regulates chromatin modifications, including H3K27me3 and ten-eleven translocation (Tet)-dependent DNA demethylation. The ability of aKG to influence epigenetic status of cells may explain both its prophylactic and anti-depressant effects since transcriptional dysregulation and aberrant epigenetic regulation are unifying themes in psychiatric disorders. This may also explain its ability to differentially regulate BDNF expression in the hippocampus and NAc.
If exercise mediates its effects through aKG, aKG may be a pivotal component of an exercise pill along with lactate and BHB that can serve as both a prophylactic and antidepressant treatment for depression.”
https://www.sciencedirect.com/science/article/pii/S266717432500031X “α-ketoglutarate (aKG) is a circulatory exercise factor that promotes learning and memory recall and has antidepressant properties