A 2025 paper performed post-hoc epigenetic clock analyses of a supplement and exercise clinical trial completed earlier this decade:
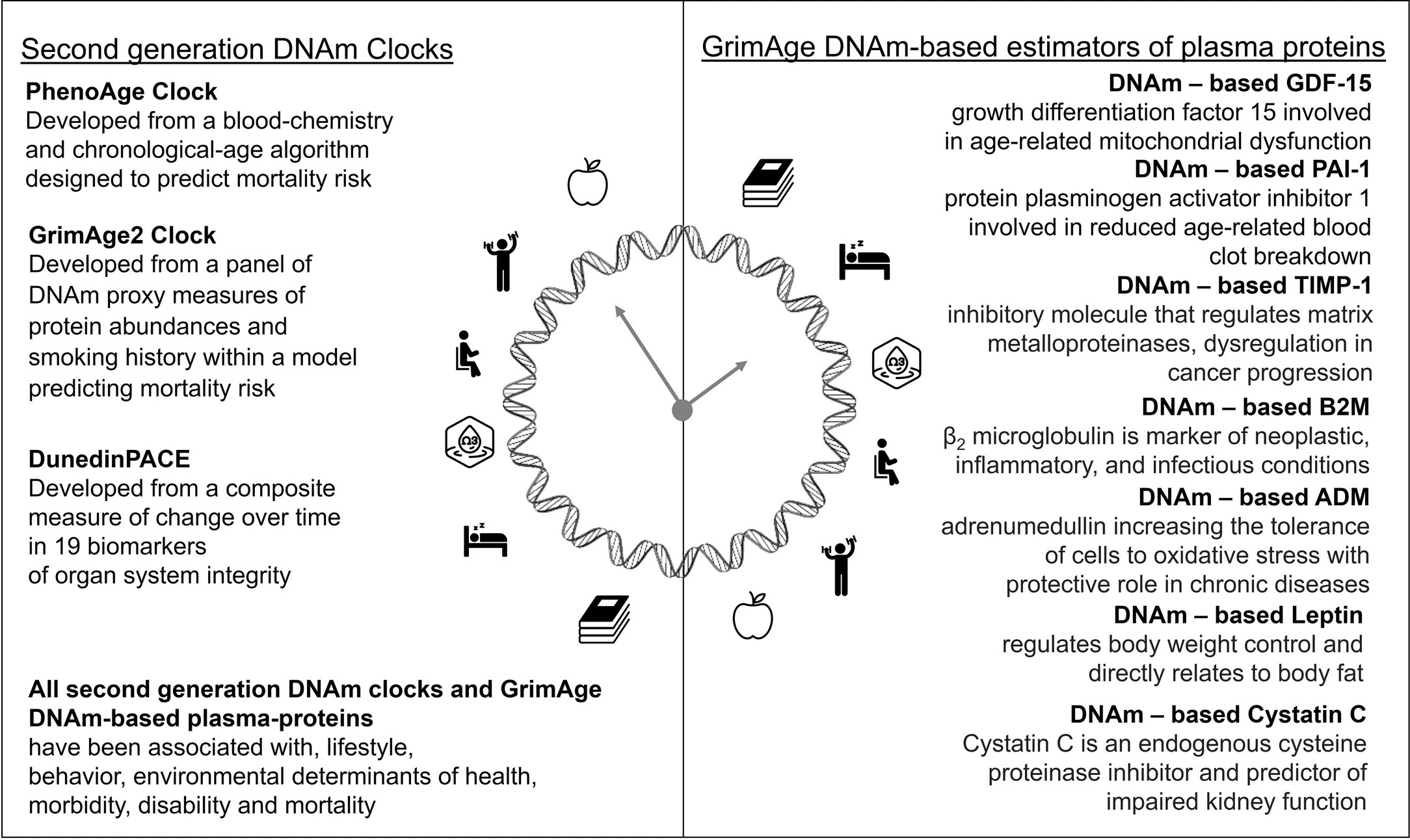
“We report results of a post hoc analysis among 777 participants of the DO-HEALTH trial on the effect of vitamin D (2,000 IU per day) and/or omega-3 (1 g (330 mg EPA plus 660 mg DHA from marine algae) per day) and/or a home exercise program (a strength-training exercise program performed for 30 min three times per week) on four next-generation DNA methylation (DNAm) measures of biological aging (PhenoAge, GrimAge, GrimAge2 and DunedinPACE) over 3 years. Omega-3 alone slowed the DNAm clocks PhenoAge, GrimAge2 and DunedinPACE, and all three treatments had additive benefits on PhenoAge.
Inclusion criteria were age 70 years and older, living at home, having no major health events (no cancer or myocardial infarction) in the 5 years before enrollment, having sufficient mobility to visit the study centers without help and having good cognitive function with a Mini-Mental State Examination score of at least 24. 777 provided consent for these analyses and had samples available after the application of the exclusion criteria. This group of individuals formed our analysis sample, which had the following characteristics: 59% were women; the mean age at baseline was 75 years; 30% had 25-hydroxyvitamin D (25(OH)D) levels of <20 ng ml−1; 53% were healthy agers as defined in the Nurses’ Health Study (free of major chronic diseases, disabilities, cognitive impairments and mental health limitations); and 88% were physically active (29% were active one to three times per week, and 59% were active more than three times per week). The Swiss participant subgroup represents a healthier and more active subgroup within the total DO-HEALTH population.
Overall, from baseline to year 3, standardized effects ranged from 0.16 to 0.32 units (2.9–3.8 months). In summary, our trial indicates a small protective effect of omega-3 treatment on slowing biological aging over 3 years across several clocks, with an additive protective effect of omega-3, vitamin D, and exercise based on PhenoAge.”
https://www.nature.com/articles/s43587-024-00793-y “Individual and additive effects of vitamin D, omega-3 and exercise on DNA methylation clocks of biological aging in older adults from the DO-HEALTH trial”
These epigenetic clock measurements of a subset of trial subjects was interesting, although I didn’t find it particularly relevant to what I do. I take twice as much Vitamin D and omega-3s everyday, do resistance exercises once or twice a week whenever I’ve recovered from the previous session, walk a few miles on the beach if the weather is nice, and other things.
I don’t bother with epigenetic clock measurements anymore because the free one (PhenoAge) is too variable to be personally accurate. For other clocks, it would be meaningless if all I got was a 2-3 month improvement over a three year period like this trial. Studies usually find that the most deficient subjects at the beginning are the ones that show the greatest improvements with effective treatments. Unhealthiness on any epigenetic clock parameter probably wouldn’t be my starting point, so I may not show even a one-month improvement over three years.
Dr. Goodenowe offered his opinion on the paper:
“DHA is a polyunsaturated fatty acid that is essential for maintaining youthful fluidity of the body’s membranes. While our bodies can make DHA from the essential omega-3 dietary fatty acid, as we get older, our ability to make DHA decreases and oxidative stress on our bodies increases. These two factors contribute to our membranes becoming stiffer and less pliable as we age, in other words, ‘older.’
Because getting older and losing function appear to go hand in hand, we equate aging with a loss of function. As such, we think that aging causes this loss of function, like a disease. Instead, the opposite is true, and it’s the loss of function that causes aging. To slow aging you need to focus on maintaining function.”
https://www.prevention.com/health/a63850396/vitamin-exercise-boost-longeivty-study/ “Scientists Find Taking This Vitamin Boosts Longevity, Add Years to Your Life”
Prevention magazine’s editors need to better proof their writers’ work before it gets published. Unlike the headline, the trial had nothing to do with adding years to human lifespan.