A trio of papers on betaine, the first being a 2021 series of thorough rodent experiments relating betaine and gut microbiota, and cause and effect:
“Compared with lean individuals, adipose tissues in obese individuals secrete high levels of pro-inflammatory cytokines such as TNF-α, IL-1β, and IL-6, inducing:
- Systemic inflammation;
- Insulin resistance;
- Large amounts of carcinogenic factors; and
- Increasing risk of certain types of cancer such as melanoma, colon cancer, and liver cancer.
Prebiotics obtained from fruits and vegetables can regulate host lipid metabolism and glucose homeostasis by reversing gut dysbiosis in obese individuals.
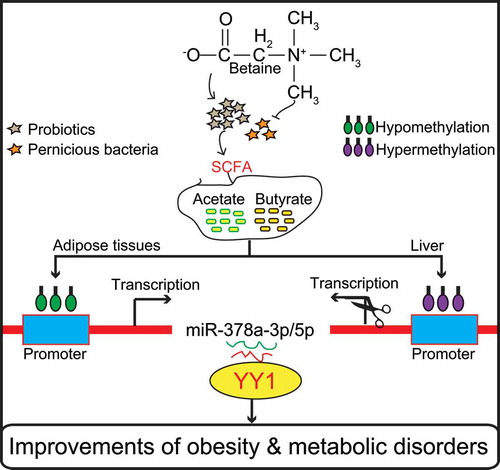
Results of this study show that dietary betaine alleviated gut microbiota imbalance in obese mice, and reduced development of obesity and obesity-related complications. Regulation of the miR-378a-YY1 regulatory axis by gut microbial acetate and butyrate was a critical mechanism for modulating:
- White adipose tissue browning;
- Classical brown adipose tissue activation; and
- Lipid and glucose homeostasis
in obese mice after betaine supplementation.
These findings offer novel insights into underlying mechanisms by which gut microbiota affect host metabolism and host immune system, and demonstrate that the betaine-gut microbiota-derived signal axis is a potential therapeutic target in obesity and metabolic syndrome.”
https://www.tandfonline.com/doi/full/10.1080/19490976.2020.1862612 “Dietary betaine prevents obesity through gut microbiota-drived microRNA-378a family”
A second 2021 paper was a meta-analysis of effects on human cardiovascular biomarkers:
“Betaine supplementation had a significant effect on concentrations of:
- Betaine;
- Total cholesterol;
- Low-density lipoprotein (LDL);
- Homocysteine [negative effect]; and
- Methionine.
Betaine supplementation did not affect serum concentrations of:
- Triglycerides;
- High-density lipoprotein (HDL);
- Fasting blood glucose;
- C-reactive protein;
- Liver enzymes alanine aminotransferase (ALT), aspartate aminotransferase (AST), gamma-glutamyl transferase (GGT); and
- Blood pressure.
Our meta-analysis supports the advantage of a lower dose of betaine supplementation (<4 g/d) on homocysteine concentrations without the lipid-augmenting effect observed with a higher dosage.”
https://www.tandfonline.com/doi/abs/10.1080/10408398.2021.1902938 “Effects of betaine supplementation on cardiovascular markers: A systematic review and Meta-analysis” (not freely available)
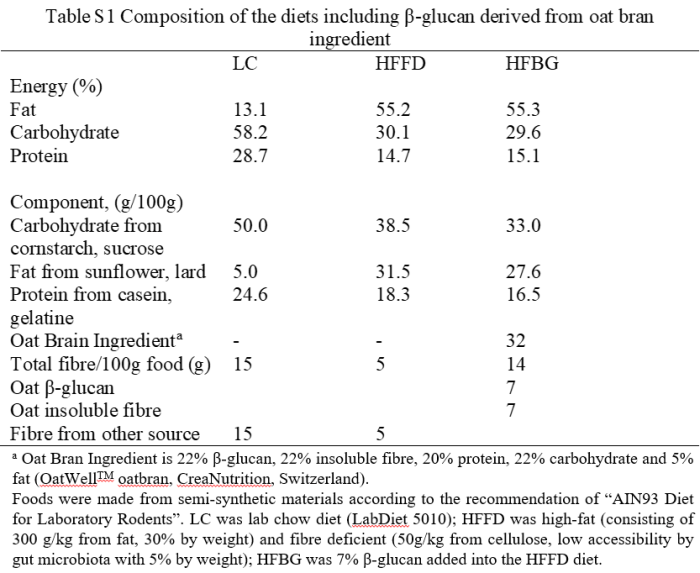
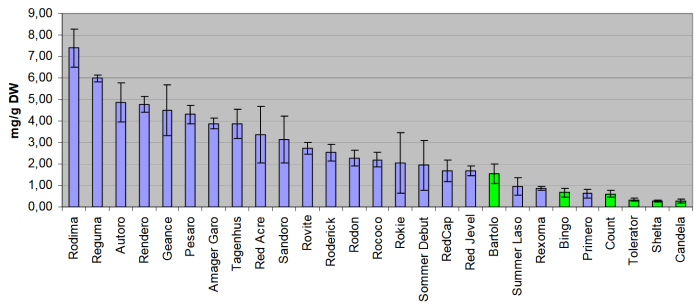
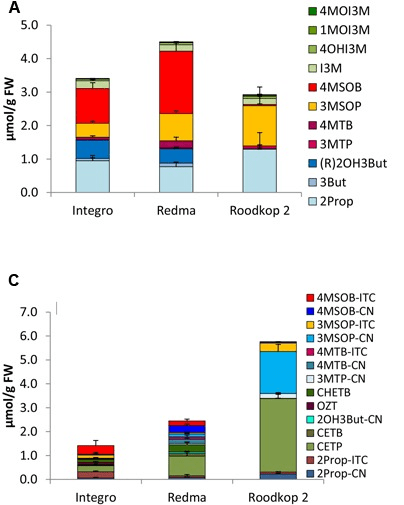
A third paper was a 2014 cereal analysis of betaine and its precursor choline that found a 224% increase in betaine from 62 to 139 μg/g and a 31% increase in choline from microwaving oats:
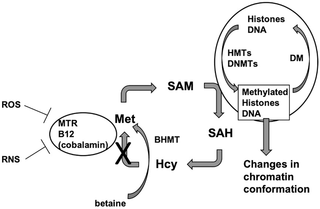
“Betaine and its precursor choline are important components of one-carbon metabolism, remethylating homocysteine into methionine and providing methyl groups for DNA methylation. Cereals are the main source of betaine in diet.
During cooking processes which did not involve removal of water (in this case oat porridge microwaved using instant oats) appeared to lead to creation of betaine. Explanations for this phenomenon could be that betaine is synthesised during the process, or that heating with water liberates betaine from cereal matrix, enhancing efficiency of extraction.”
https://www.sciencedirect.com/science/article/abs/pii/S0308814613012247 “Cereal foods are the major source of betaine in the Western diet – Analysis of betaine and free choline in cereal foods and updated assessments of betaine intake” (not freely available)
Another 2021 betaine (aka trimethyl glycine) study was curated in Ride the waves of gene expression with betaine for its role in preventing nerve disease. I take 1.5 grams of a betaine supplement every morning and evening when eating hulled Avena sativa 3-day-old oat sprouts.
I found the first two papers from their citing a 2016 human and rodent study Dietary Betaine Supplementation Increases Fgf21 Levels to Improve Glucose Homeostasis and Reduce Hepatic Lipid Accumulation in Mice, which was linked in a comment on this 2021 video: