This 2021 rodent study investigated effects of four different types of dietary fiber on two different types of aged human microbiota:
“Individual differences in gut microbiota may influence host metabolic responses to dietary fiber in humans. Dietary fibers are edible carbohydrates resistant to host digestive enzymes, and not broken down or absorbed in the small intestine.
We colonized genetically identical germ-free mice with two distinct human fecal communities and fed them isocaloric diets containing different types of fiber. We used fecal specimens from a cohort of previously analyzed samples obtained from adults in their mid-seventies.
We used 10% dietary fiber and 35% kcal derived from fat as comparable to the intake level of dietary fiber in US adults:
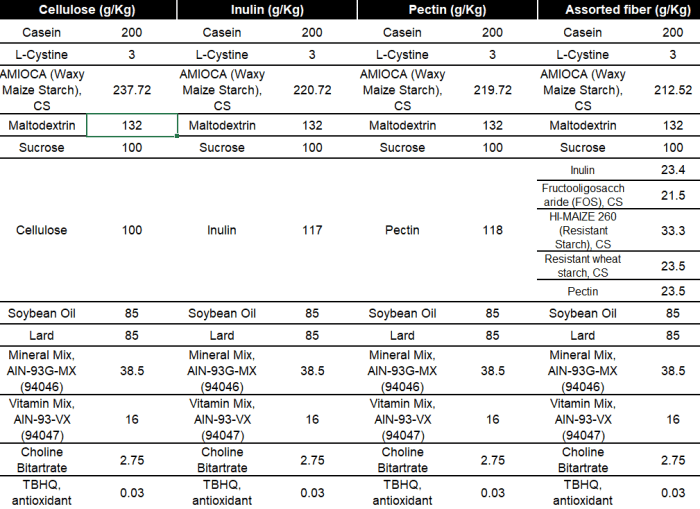
All mice had the same assorted fiber diet for two weeks. Mice were then switched to one of four diets described above: cellulose, inulin, pectin, and assorted fiber, and maintained in these diets for another 4 weeks.
There was a ~ 4-fold range in levels of cecal butyrate among the eight groups despite all animals consuming the same diet [before switching]. Butyrate is known to vary widely among humans and has been linked with beneficial health effects on the host:

We chose inulin and pectin as the former is commonly used as a prebiotic, while the latter has been proven to support growth of a wide variety of gut microbes, and it is commonly used as a dietary supplement. We also chose these two dietary fibers due to their distinct structures, including differences in basic units, linkages, and degree of polymerization.
Assorted fiber diet had the same total amount of dietary fiber as treatment groups used in this study, but with more diversity [FOS and two resistant starches] in fermentable substrates, which we reasoned would support engraftment of taxa relevant to all dietary treatments. Inclusion of this group in the experimental phase also served as a control to inform whether this diet used during colonization drove major differences.
Diet and its interaction with gut community showed a significant effect on serum glucose levels. While pectin diet had an overall beneficial effect on metabolic phenotypes relative to non-fermentable cellulose for SubA-colonized mice, this diet was less favorable for SubB-colonized animals, which showed the strongest benefits on inulin fiber.
In inulin diet, mice inoculated with SubB showed decreased adiposity, decreased liver triglycerides (TG) and lower serum levels of fasting glucose relative to animals colonized with SubA. In contrast, pectin-fed mice colonized with SubB accumulated more fat mass relative to SubA-colonized counterparts, whereas serum glucose and liver TG were comparable between the two community groups.
Mice colonized with SubB showed significantly lower levels of adiposity than those colonized with SubA in the assorted fiber diet, whereas serum glucose and liver TG were comparable.
We found that these two transplanted communities elicited divergent metabolic epigenetic and transcriptional responses to the same dietary fiber. Furthermore, differences between mice colonized with these two communities varied depending on type of fiber consumed.
Populations contain a significant amount of genetic variation derived from their largely individual associated microbiomes. Dissecting effects of gut microbial vs. host genetic variation while controlling environmental exposure is practically impossible to achieve in human studies.
One-size-fits-all approaches to promote health are unlikely to elicit consistent effects across individuals. Identifying gut microbial biomarkers associated with beneficial responses to common interventions may help to stratify subjects into more effective personalized treatments.”
https://microbiomejournal.biomedcentral.com/articles/10.1186/s40168-021-01061-6 “Gut microbiome variation modulates the effects of dietary fiber on host metabolism”
1. This study nailed it! You are what you eat, and The future of your brain is in your gut right now.
2. Group differences in cecal butyrate in the second graphic were instructive. But what really needed to be analyzed was each individual subject’s responses within the eight groups, and each individual’s characteristics.
What did or didn’t matter to each individual could then be applied and analyzed to what did or didn’t matter to its group. Researchers need to flip from a top-down statistics-package approach, to a bottoms-up individual paradigm for evidence.
3. Haven’t mentioned Increasing soluble fiber intake with inulin recently. I eat the labeled 2.5 grams serving. More than that runs into a 10 g “Over this dose would induce mild gastrointestinal symptoms” threshold.
I eat a half-dozen cloves of garlic in daily AGE-less chicken vegetable soup. Garlic contains ≈ 16% inulin, contributing 4-5 g inulin.
4. My dietary fiber intake of current practices is well beyond this study’s 10%. Several times more than our human ancestors’ estimated 100 g/day if Switch on your Nrf2 signaling pathway measurements are correct?
Trying to make my gut microbiota happy, expecting that they’ll reciprocally respond. Dietary fat content is < 10 %.
I also aim for a high fiber diet. Since we briefly mentioned Dr. Lustgarten, he has written a lot about a high fiber diet and butyrate-producing strains. Here one of his publications with that regard: https://www.researchgate.net/publication/339882131_Investigation_of_the_Diet-Gut-Muscle_Axis_in_the_Osteoporotic_Fractures_in_Men_Study
What I mean to remember though, is that Dr. Lustgarten had his intestinal microbiome sequenced, and even though he had aimed for a very high fiber diet for years he was still disappointed about the numbers of butyrate-producing strains he appeared to have. I can’t find this post of him anymore though.
Personally I think more interventions may be needed than solely dietary interventions in subjects that had repeated and longer courses of antibiotics in their lifetime.
Watched his May 3, 2020, video Optimizing Biological Age over the weekend. He said something to the effect that he doesn’t eat grains, relying on fiber of 100 grams from mainly vegetables.
“500g of broccoli, 500g cauliflower, ~150g beets, ~150g spinach, 20g parsley, ~400g carrots, ~330g red bell peppers” from his pneumonia video comments. I do both grains and vegetables.
The site he recommends for fiber content https://www.prebiotin.com/pages/fiber-explained has their definitions mixed up. Maybe to sell their product?
Fiber isn’t the binary insoluble and soluble that site presents. Insoluble, indigestible, non-fermentable fiber by the entire gastrointestinal tract like cellulose has null effects, unlike indigestible by stomach and small intestine but fermentable by colon microbiota fiber like FOS, GOS, inulin, etc.
Whole wheat was listed, but not whole oats. That’s fine because that site would have conflated my breakfast’s soluble β-glucan 1,3/1,4 content with indigestible yet fermentable Avena nuda whole oat components.
Had to back off sprouting separate 10.7 g broccoli, red cabbage, and mustard batches twice daily in favor of one combined 10.7 g batch because the extra 4.6 oz. twice daily 3-day-old sprouts were too much fiber for me. Still sprout 20 g hulled Avena sativa oats twice daily, which become 51.9 g after three days.
Pretty sure I’m well over 100 g fiber, but don’t know because I don’t measure. What I feel matters, not a third-party’s misaligned measurements.
Thanks for the fantastic info. I added wheat germ the past months for spermidine as mentioned, and I am going to add the sprouted oats upon reading your articles.