This 2021 rodent study investigated oat β-glucan effects on colitis:
“In this study, we determined effects of consumption of low- and high-molar-mass oat beta-glucans on expression of selected markers of apoptosis and autophagy in colonocytes in TNBS colitis-induced rats. We analyzed expression of colon wall receptors, including TLRs and Dectin-1, which are involved in recognition of molecular patterns of pathogens in colon epithelial cells.
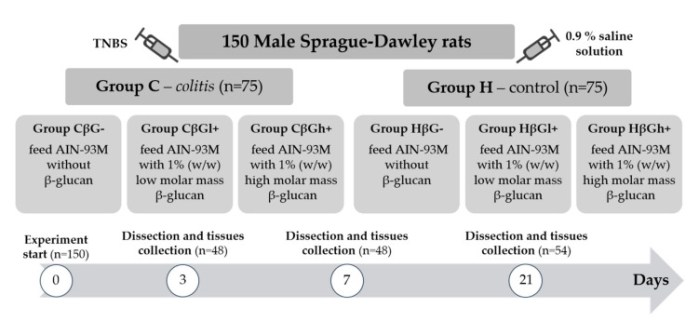
Rats were divided into two main groups: healthy control (H) and a TNBS (2,4,6-trinitrobenzosulfonic acid)-induced colitis (C) group, both including subgroups fed feed without beta-glucans (βG−) or feed supplemented with low- (βGl) or high-molar-mass oat beta-glucans (βGh) for 3, 7, or 21 days. Expression of autophagy (LC3B) and apoptosis (Caspase-3) markers, as well as Toll-like (TLRs) and Dectin-1 receptors in colon epithelial cells, was determined.
1. [Autophagy] Autophagy contributes to adaptation of cells and maintenance of intracellular homeostasis enabling cells to survive under stressful conditions. The autophagy marker in colon wall and intestinal epithelial cells (IECs) investigated was expression of LC3B protein, which participates in formation and maturation of autophagosomes.
A decrease in this protein was found in colon wall after TNBS administration, which indicates intense repair processes of intestinal epithelium accompanying / preceding the period of Crohn’s disease (CD) remission. The above data indicate a significant effect of oat beta-glucans in restoring autophagy in inflamed IECs, and a stronger effect of oat beta-glucans with a high molar mass, which also increased activity of autophagy in colon tissue of control animals without colitis.
2. [Apoptosis] In early development of acute colitis, expression of Caspase-3, the executive enzyme of apoptosis, was very low. The highest expression of Caspase-3 protein was observed in control (HβGh+), feed supplemented with high-molar-mass oat beta-glucans.
- After 7 days of TNBS administration, Caspase-3 expression in colitis-induced animals was approximately eight times higher than in control group, which indicates an increase in apoptosis in response to intestinal inflammation.
- Consumption of feed supplemented with high-molar-mass oat beta-glucans by colitis animals resulted in approximately two times lower Caspase-3 expression after 7 days. Physical properties of high-molar-mass beta-glucans favor formation of a protective layer on inner wall of intestine, effectively supporting development of beneficial microbiota producing short-chain fatty acids.
- Consumption of feed with low-molar-mass oat beta-glucans resulted in expression of this enzyme in colitis animals at a similar level as in control group.
This confirms significant effect of oat beta-glucans in reducing expression of Caspase-3 during ongoing inflammation, with low-molar-mass beta-glucans having a stronger effect.
3. [Dectin-1] Expression of Dectin-1 across all experimental time points was found to be reduced due to induced inflammation. We analyzed Dectin-1 expression in intestinal epithelial cells, not in colon wall or immune cells. Decrease in Dectin-1 expression in colonocytes noticed in our study may be related to disrupted intestinal barrier integrity by the ethanolic TNBS solution, that as a consequence, causes infiltration of pathogens / antigens into deeper layers of colon wall and allows their direct contact with cells of the immune system.
Results showed an increase in expression of Dectin-1 in inflamed IECs under influence of oat beta-glucans. A similar effect on expression of LC3B protein was noted, with oat beta-glucans of a high molar mass having a stronger effect.
4. [TNF-α] Concentration of TNF-α and other proinflammatory cytokines in colon wall of animals with TNBS-induced inflammation was significantly increased at all time points. Consumption of oat beta-glucans reduced concentration of these inflammatory factors.
The extrinsic pathway of apoptosis is induced by binding of this factor to the TNFR1a receptor. Increased autophagy in inflamed intestinal epithelium protected cells against TNF-α-induced apoptosis, which in turn helped to maintain integrity of the intestinal barrier and reduce inflammation.
5. [TLRs] After 3 days of TNBS administration, expression of TLR 4 and TLR 6 receptors in colonocytes was significantly lower in the colitis group receiving feed without beta-glucans as compared to control group. In the same group of rats (CβG−), TLR 5 expression was lower.
Decrease in expression of these receptors is mostly influenced by acute intestinal inflammation. Oat beta-glucans caused a significant increase in expression, especially TLR 5 and TLR 6, in inflamed IECs.
In summary, oat beta-glucans were found to alleviate the course of induced inflammation.”
https://www.mdpi.com/2072-6643/13/2/321/htm “Effects of Dietary Oat Beta-Glucans on Colon Apoptosis and Autophagy through TLRs and Dectin-1 Signaling Pathways – Crohn’s Disease Model Study”
Eat oats to prevent inflammatory diseases:
“Oat beta-glucans with a high molar mass increased activity of autophagy in colon tissue of control animals without colitis.”
If we don’t do that, eat oats to treat inflammation:
“Confirms significant effect of oat beta-glucans in reducing expression of Caspase-3 during ongoing inflammation, with low-molar-mass beta-glucans having a stronger effect.”
I eat primarily low- and medium-molecular-weight oat β-glucan twice a day with 3-day-old hulled Avena sativa oat sprouts. For breakfast I eat primarily high-molecular-weight oat β-glucan in hulless Avena nuda oats soaked 16+ hours and microwaved 20 minutes at 80% power in a 1000W microwave.
An oats β-glucan clinical trial tested low-, medium-, and high-molecular-weight oat β-glucan in 14 people. It found:
“Bioprocessing of oat bran with enzyme treatment, causing depolymerization of β-glucan, affects nutritional properties of bran and functional properties of β-glucan in human gastrointestinal tract.”
Neither study investigated gut microbiota. Pretty sure our hosted microorganisms had roles in both studies’ findings.
See the third paper of Reinforce your immune memory every day for a related 2021 rodent study.