Two papers on Vitamin K, beginning with a 2021 review:
“Vitamin K is involved in many biological processes. Menaquinones (MK) [Vitamin K2] and phylloquinone [Vitamin K1] vary in biological activity, showing different bioavailability, half-life, and transport mechanisms.
The effective dose to decrease uncarboxylated osteocalcin was six times lower for MK-7 than for MK-4. Similarly, MK-7 affected blood coagulation system at dose three to four times lower than vitamin K1.
Both vitamin K1 and MK-7 inhibited decline in bone mineral density. However, benefits for occurrence of cardiovascular diseases have been observed only for long-chain menaquinones. There are currently no guidelines for recommended doses and forms of vitamin K in prevention of osteoporosis, atherosclerosis, and other cardiovascular disorders.”
https://www.mdpi.com/2304-8158/10/12/3136/htm “Relationship between Structure and Biological Activity of Various Vitamin K Forms”
This first paper cited a 2019 meta-analysis for:
“Vitamin K2 supplementation is a preventative measure rather than an osteoporosis treatment.
Meta-analysis of various interventions for improving BMD revealed that vitamin K2 can increase lumbar spine BMD. It ranked sixth among eighteen different single or combined interventions including Ca, vitamin D, estrogen, isoflavone and exercise.
Effect size for change in bone mineral density (BMD) using forest plots. LS, lumbar spine; D, vitamin D; Est, oestrogen; Ex, exercise; K, vitamin K; Iso, isoflavone; FN, femoral neck.
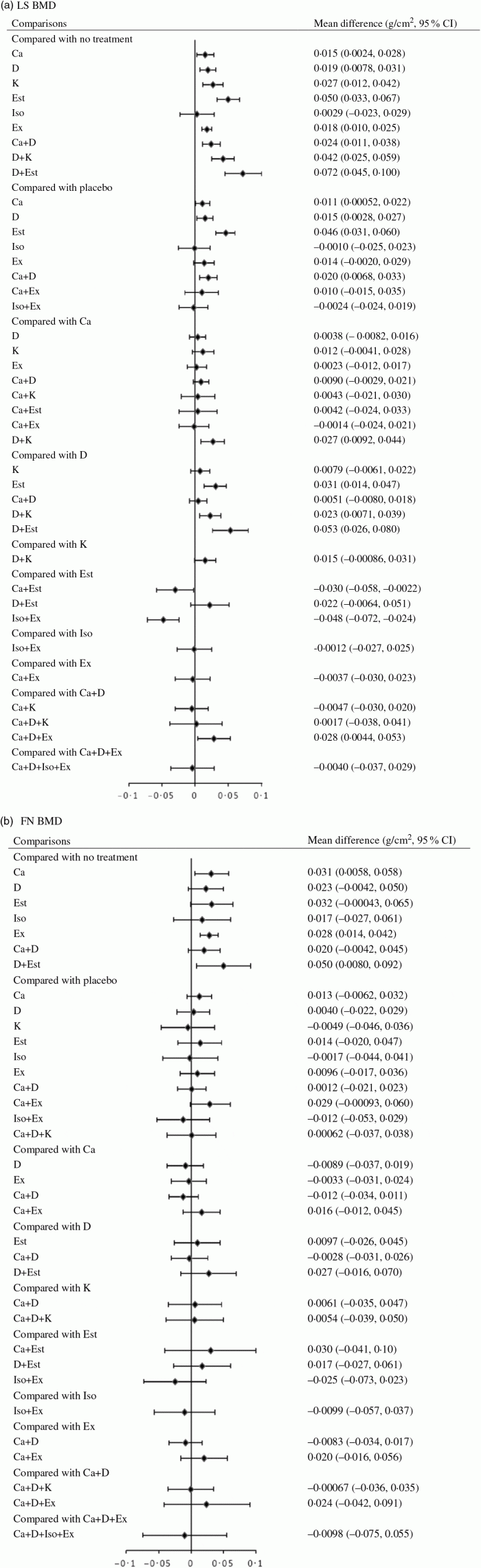
Lumbar spine:
- Ca, vitamin D, vitamin K, oestrogen, exercise, Ca + vitamin D, vitamin D + vitamin K, and vitamin D + oestrogen were associated with significantly beneficial effects relative to no treatment.
- Ca, vitamin D, oestrogen, and Ca + vitamin D were associated with beneficial effects compared with placebo.
- Vitamin D + vitamin K was associated with positive effect with Ca.
- Oestrogen, vitamin D + vitamin K, and vitamin D + oestrogen were associated with beneficial effect compared with vitamin D.
- Ca + vitamin D + exercise had a beneficial effect compared with Ca + vitamin D.
- Ca + oestrogen, and isoflavone + exercise were related to negative effects relative to oestrogen.
Femoral neck:
- Ca, exercise, and vitamin D + oestrogen were associated with significant beneficial intervention effects relative to no treatment.
The present study demonstrated that many interventions were valuable for improving BMD in the LS and FN of postmenopausal women. It confirmed the need for postmenopausal women to improve BMD through preventive measures such as nutrients or oestrogen.
It also confirmed that different single or combined preventions can affect BMD at different sites in different orders. This reveals to medical and health workers and postmenopausal women which methods can be selected preferentially to prevent bone loss.”
https://doi.org/10.1017/S0007114519002290 “Impact of calcium, vitamin D, vitamin K, oestrogen, isoflavone and exercise on bone mineral density for osteoporosis prevention in postmenopausal women: a network meta-analysis”
Amazingly oblivious that this freely-available second 2019 paper has been cited only by this first paper. What recent literature is more relevant to postmenopausal women’s health?